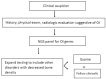
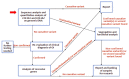
Clinical Description
The severity of COL1A1/2 osteogenesis imperfecta (COL1A1/2-OI) ranges from perinatal lethality to individuals with severe skeletal deformities, mobility impairments, and very short stature to nearly asymptomatic individuals with a mild predisposition to fractures, normal stature, and normal life span.
COL1A1/2-OI is classified into four more common types based on clinical presentation, radiographic features, family history, and natural history [Sillence et al 1979]. An update of the Sillence classification has been proposed and has gained some acceptance [Emery & Rimoin 2012]. Although this classification of COL1A1/2-OI into types is helpful in providing information about prognosis and management of a given individual, the features of different types of COL1A1/2-OI overlap and it is not always easy to categorize the extent of the clinical disorder. It is helpful to remember that the severity of clinical and radiographic features lies on a continuum and that the "types" are defined using characteristics that appear to form clinical "nodes." Interfamilial variability is apparent among individuals with the same OI type and intrafamilial variability is apparent among individuals with the same causative variant. Nonetheless, it is reasonable to continue to think of COL1A1/2-OI in terms of these types in order to provide information about the expected natural history of the disorder.
Classic non-deforming OI with blue sclerae (previously OI type I) is characterized by blue sclerae and normal stature. A small proportion of infants with OI type I have femoral bowing at birth. The first fractures may occur at birth or with diapering. More often, the first fractures occur when the infant begins to walk and, more importantly, to fall. Fractures generally occur at a rate of a few to several per year and then decrease in frequency after puberty. Fracture frequency often increases again in adulthood, especially in postmenopausal women and men beyond the fifth decade [Paterson et al 1984]. Affected individuals may have anywhere from a few fractures to more than 100, but the fractures usually heal normally with no resulting deformity.
Most affected individuals have normal or near normal stature but are often shorter than other members of their families and shorter than predicted based on parental heights.
Joint hypermobility predisposes to a number of minor comorbidities. The primary clinical concern is early-onset degenerative joint disease due to malalignment of articular surfaces.
In their classification of OI, Sillence et al [1979] designated a subset of classic non-deforming OI with dentinogenesis imperfecta (DI) (OI type IB). In individuals with DI, morbidity results not from dental decay but rather from premature wearing down of the teeth. DI can be a significant cosmetic concern. Dental eruption in classic non-deforming OI can sometimes occur early.
Progressive hearing loss occurs in about 50% of adults with classic non-deforming OI, beginning as a conductive hearing loss but often with an additional sensorineural hearing loss component in time.
Perinatally lethal OI (previously OI type II). Abnormalities characteristic of perinatally lethal OI are evident at birth. Weight and length are small for gestational age. The sclerae are dark blue and connective tissue is extremely fragile. The skull is large for the body size and soft to palpation. Callus formation on the ribs may be palpable. Extremities are short and bowed. Hips are usually flexed and abducted in a "frog-leg" position. Although some fetuses with perinatally lethal OI die in utero or are spontaneously aborted, more typically infants die in the immediate perinatal period. More than 60% of affected infants die on the first day; 80% die within the first week; survival beyond one year is exceedingly rare and usually involves intensive support such as continuous assisted ventilation [Byers et al 1988]. Death usually results from pulmonary insufficiency related to the small thorax, rib fractures, or flail chest because of unstable ribs. Those who survive the first few days of life may not be able to ingest sufficient calories because of respiratory distress.
Histologic evaluation of bone from infants with perinatally lethal OI shows marked reduction in collagen in secondary trabeculae and cortical bone [Horton et al 1980]. Cortical bone is hypercellular with large osteocytes. Trabeculae contain woven bone with large immature osteoblasts [Cole et al 1992, Cole & Dalgleish 1995].
Progressively deforming OI (previously OI type III). The diagnosis of progressively deforming OI is readily apparent at birth. Fractures in the newborn period, simply with handling of the infant, are common. In some affected infants, the number and severity of rib fractures lead to death from pulmonary failure in the first few weeks or months of life.
Infants who survive this period generally fare well, although most do not walk without assistance and usually use a wheelchair or other assistance for mobility because of severe bone fragility and marked bone deformity. Affected individuals have as many as 200 fractures and progressive deformity even in the absence of obvious fracture. Progressively deforming OI is often difficult to manage orthopedically, even with intramedullary rod placement.
Growth is extremely delayed and adults with progressively deforming OI are among the shortest individuals known, with some having adult stature of less than one meter.
Intellect is normal unless there have been intracerebral hemorrhages (extremely rare). Faqeih et al [2009] published a report identifying increased risk for intracranial hemorrhage (ICH) in a "small number" of individuals who were identified to have pathogenic variants affecting exon 49 of COL1A2, which codes for the most carboxy-terminal part of the triple-helical domain of the collagen alpha-2(I) chain. They concluded that this pathogenic variant appeared to increase the risk for abnormal limb development and intracranial bleeding. Budsamongkol et al [2019] reported a young boy with marked joint hypermobility, significant DI, brachydactyly, and a COL1A2 pathogenic variant found to be associated with ICH by Faqeih et al [2009]. The boy had not experienced an ICH, but as some of the original affected individuals only presented with ICH in their teenage years, this does not eliminate the risk in this young individual.
Even within progressively deforming OI, considerable heterogeneity is observed at the clinical level. Some individuals have normal-appearing teeth and facies while others have DI, a large head, and enlarged ventricles that reflect the soft calvarium. Relative macrocephaly and barrel chest deformity are observed. Usually sclerae are blue in infancy but lighten with age. Hearing loss generally begins in the teenage years. As molecular testing of this subgroup further differentiates those with COL1A1/2-OI from the autosomal recessive forms, the clinical profile of this heterogeneous group will become more refined.
Basilar impression, an abnormality of the craniovertebral junction caused by descent of the skull on the cervical spine, is common. Basilar impression is characterized by invagination of the margins of the foramen magnum upward into the skull, resulting in protrusion of the odontoid process into the foramen magnum. Basilar impression may progress to brain stem compression, obstructive hydrocephalus, or syringomyelia because of direct mechanical blockage of normal CSF flow [Charnas & Marini 1993, Sillence 1994, Hayes et al 1999]. Symptoms of basilar impression become apparent with neck flexion. Findings include posterior skull pain, C2 sensory deficit, tingling in the fourth and fifth digits, and numbness in the medial forearm. When swimming, affected individuals may perceive that water temperature differs below and above the umbilicus. Lhermitte's sign (tingling on neck flexion) can be demonstrated at any stage. Basilar impression can cause headache with coughing, trigeminal neuralgia, loss of function of the extremities, or paresthesias. At its most severe involvement, sleep apnea and death can occur.
Common variable OI with normal sclerae (previously OI type IV) is characterized by mild short stature, DI, adult-onset hearing loss, and normal-to-gray sclerae. This is the most variable form of OI, ranging in severity from moderately severe to so mild that it may be difficult to make the diagnosis.
Stature is variable and may vary markedly within the family. DI is common but may be mild. Sclerae are typically light blue or gray at birth but quickly lighten to near normal. Hearing loss occurs in some and basilar impression can occur.
Other Considerations
Facial features. Infants and children with OI are often described as having a triangular face. The skull is relatively large compared to body size.
Other skeletal problems. Individuals with OI may also have scoliosis, early-onset arthritis, non-inflammatory arthralgia, and myofascial pain.
Skin. Easy bruising is a frequent observation in individuals with OI. This is believed to be caused by microvascular fragility and poor microstructural support of the connective tissues.
Hearing loss. Mixed conductive and sensorineural hearing loss afflicts the majority of adults with OI. Childhood-onset hearing loss affects approximately 7% of affected children between ages five and nine years; progressive postpubertal hearing loss is more typical. The initial conductive hearing loss results from fractures of the bones of the middle ear with contracture and scarring of the incus. With age, sensorineural hearing loss compounds the preexisting conductive element. Fixation of the stapes is not unlike otosclerosis and surgical techniques such as stapedotomy used to treat otosclerosis have shown similar success in treating hearing loss in OI [van der Rijt & Cremers 2003, Kuurila et al 2004, Doi et al 2007]. Bisphosphonate therapy has not been shown to influence hearing loss.
Gastrointestinal. Although complaints of constipation are common in adults with OI who are mobile in wheelchairs, it is not clear if this is a complication of OI itself or of the mode of transport. Bowel obstruction can occur as a result of protrusio acetabuli [Lee et al 1995] but appears to be uncommon.
Cardiovascular. Emerging data support an increased risk for cardiac and vascular disease in OI. Ashournia et al [2015] performed a systematic review of the literature in 2015 documenting a broad array of cardiovascular phenotypes with higher prevalence in individuals with a clinical diagnosis of OI including arterial and aortic dissection. Balasubramanian et al [2019] reported three additional individuals with COL1A1/2-OI and aortic aneurysms. There is still no consensus on cardiovascular surveillance, although some centers have initiated screening echocardiograms every three to five years to monitor for this risk.
Development. Cognition is expected to be normal but gross motor development may be hindered by joint hypermobility and progressive deformity due to recurrent fractures.
Functional limitations. Individuals with OI may experience other functional limitations, although these will be highly dependent on the specific physical manifestations of OI.
Life expectancy. The severely affected neonates with perinatally lethal OI typically do not survive, with a significant proportion of infants dying within the first 48 hours. Aggressive life support can prolong survival but ultimately the most severe forms remain perinatally lethal. Life expectancy for classic non-deforming OI and common variable OI is normal. Progressively deforming OI is highly variable and life expectancy may be shortened by the presence of severe kyphoscoliosis with attendant restrictive pulmonary disease resulting in cardiac insufficiency.
Genotype-Phenotype Correlations
It is important to keep the exceptions in mind when providing genetic counseling, particularly in the prenatal setting. Genotyping can be helpful in distinguishing classic non-deforming OI from all other types of OI.
Classic non-deforming OI almost always results from a pathogenic variant in one COL1A1 or COL1A2 allele that introduces premature termination codons and decreases the stability of mRNA (nonsense-mediated decay of the message resulting in a quantitative reduction of the collagen fibril). These causative variants may occur by codon changes, by frame shifts, and by splicing that results in use of cryptic splice sites and premature termination. The type I collagen molecule contains two pro α1(I) chains and a single α2(I) chain. If the number of available pro α1(I) chains decreases, the amount of the trimer manufactured is diminished because no more than one pro α2(I) chain can be accommodated per molecule.
Perinatally lethal OI, progressively deforming OI, and common variable OI all result from pathogenic variants that alter the structure of either pro α1(I) or pro α2(I) chains. This causes a dominant-negative effect whereby the abnormal protein is integrated into the triple helix and collagen fibril, which in turn undergoes continual remodeling, thus resulting in significantly compromised structural integrity of the bone matrix (a qualitative impact on the protein product).
The most common pathogenic variants result in substitution of another amino acid for glycine in the triple helical domain of either chain; serine, arginine, cysteine, and tryptophan result from substitutions in the first position of the glycine codon and alanine, valine, glutamic acid, and aspartic acid result from substitutions in the second position of the glycine codon. Glycine is the least bulky amino acid, and other substituting amino acids do not fit well into the collagen triple helix.
Substitutions in the pro α1(I) chain by arginine, valine, glutamic acid, aspartic acid, and tryptophan are almost always lethal if they occur in the carboxyl-terminal 70% of the triple helix and have a non-lethal but still moderately severe
phenotype if they occur in the remainder of the chain.
For the smaller side-chain residues (serine, alanine, and cysteine), the phenotypes are more variable and appear to reflect some characteristics of the stability profile of the triple helix that are not yet fully recognized.
Much more variability occurs with pathogenic variants that affect glycine residues in the pro α2(I) chain, even with the large side-chain residues; therefore, it is more difficult to determine the
genotype-
phenotype relationship.
The other common disease-causing variants affect splice sites. Variants that lead to exon skipping in the pro α1(I) chain beyond exon 14 and in the pro α2(I) chain beyond exon 25 are generally lethal. The phenotypes resulting from pathogenic variants in the upstream region are more variable and may lead to significant joint hypermobility.
A relatively small number of pathogenic variants that alter amino acid sequences in the carboxyl-terminal regions of both chains have been identified. These domains are used for chain association and pathogenic variants have the capacity to destroy this property or lead to abnormalities in chain association. The phenotypic effects of pathogenic variants that affect this domain appear to be milder when they result in exclusion rather than inclusion of the chain.
Somatic mosaicism for dominant pathogenic variants has been recognized in perinatally lethal OI, progressively deforming OI, and common variable OI. The phenotype of the individual with somatic mosaicism can range from no identifiable characteristics of OI to one of the mild forms. The current estimate for the incidence of somatic/gonadal mosaicism is up to 16% of families.
Individuals with
somatic mosaicism for variants that result in non-lethal forms of OI generally have no phenotypic features of OI, even when the variant is present in a majority of somatic cells.
Somatic
mosaicism for variants that result in lethal OI can produce a mild OI
phenotype if the variant is present in the majority of somatic cells; otherwise, the mosaicism is generally asymptomatic.